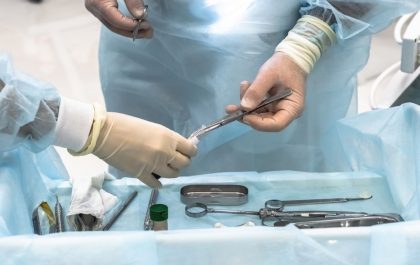
Men who are researching vasectomy reversal are usually dealing with a significant change in their circumstances – a new relationship, a lost child, or a shift in how they feel about having more children. Whatever the reason, the decision to pursue reversal is one that deserves a clear and honest picture of what the procedure involves, what the outcomes data actually shows, and what factors most influence whether it will work. Lazare Urology performs vasectomy reversals using microsurgical technique in an in-office operating room, and the questions we hear most often from New York-area men considering the procedure are the same ones this post addresses directly: how the surgery works, what time since vasectomy means for success, and what “success” actually means when fertility outcomes are more complex than a single number suggests.
Two Different Procedures, One Decision
A vasectomy reversal is not one standardized surgery. There are two distinct microsurgical procedures – vasovasostomy and vasoepididymostomy – and which one is appropriate depends on what the surgeon finds during the operation.
A vasovasostomy reconnects the two cut ends of the vas deferens directly. This is the more common of the two procedures and is appropriate when sperm are present in the fluid found in the vas deferens on the testicular side of the blockage. Under high-powered magnification, the surgeon opens both ends of the vas, examines the fluid, and if sperm are present, joins the two ends using sutures finer than a human hair. The goal is a watertight connection through which sperm can flow again.
A vasoepididymostomy is a more technically demanding procedure. It’s performed when no sperm are found in the vas deferens fluid, which can happen after a long interval since vasectomy or when backpressure from the blocked vas has caused a secondary obstruction in the epididymis – the coiled tube where sperm mature and are stored. In this case, the vas is connected directly to the epididymis, bypassing the obstruction. This procedure requires a higher level of microsurgical skill because the structures involved are significantly smaller.
The critical point is that the surgeon cannot always know in advance which procedure will be necessary. The decision is made on the operating table based on what the intraoperative assessment shows. A surgeon who can perform both and who has the microsurgical training to make that determination accurately is essential.
How Time Since Vasectomy Affects the Outcome
This is the factor that men most often want to understand, and the data is worth being precise about. The success rates for vasectomy reversal decline as more time passes since the original vasectomy, but the relationship is not linear and the decline is more gradual than many men assume.
Published data from large microsurgical series suggests the following general patterns for vasovasostomy:
In men who had a vasectomy fewer than 3 years before reversal, patency rates (sperm returning to the ejaculate) are reported above 95% in experienced hands. Pregnancy rates in those series are in the 75% range.
For vasectomies performed 3 to 9 years before reversal, patency rates remain high – generally above 85-90% – with pregnancy rates around 53-55%.
At 9 to 14 years, patency rates are still meaningful – roughly 79-80% – though pregnancy rates drop to the 40s.
Beyond 15 years, vasovasostomy patency rates drop more substantially, and vasoepididymostomy becomes more likely to be needed. Pregnancy rates for reversals in this timeframe are lower, though not zero, and individual results vary considerably.
These figures come from high-volume microsurgical series and represent outcomes from experienced surgeons. They are directionally useful, but they are not guarantees. Each patient’s anatomy, the partner’s fertility status, and the technical findings at surgery all contribute to the actual outcome.
The Difference Between Patency and Pregnancy
This distinction matters and isn’t always made clearly in patient-facing content. Patency means that sperm have returned to the ejaculate – the reversal was surgically successful. Pregnancy is a different outcome, one that depends on factors beyond the reversal itself: the partner’s age and fertility, how frequently the couple is trying to conceive, and how much time has passed since the reversal before a pregnancy attempt.
A man who is 45 reversing a 12-year-old vasectomy to conceive with a 40-year-old partner is in a very different position than a 35-year-old reversing a 5-year-old vasectomy with a 32-year-old partner, even if the surgical outcomes are comparable. The reversal is one component of the fertility picture, not the whole picture.
This is worth raising before the procedure because it affects how realistic expectations should be set and whether IVF with sperm extraction might be discussed as a parallel or alternative path. A urologist who is honest about this distinction provides better preoperative counseling than one who presents reversal as a straightforward fix without engaging the complexity.
What Recovery From a Vasectomy Reversal Looks Like
Vasectomy reversal is a more involved procedure than the original vasectomy. It typically takes 2-4 hours under sedation and involves a higher degree of technical precision. Recovery reflects that.
Most men plan for about a week of reduced activity, avoiding anything that strains the scrotal area or elevates heart rate significantly. Scrotal support and intermittent ice are standard for the first few days. Discomfort is manageable with over-the-counter pain medication for most patients.
Return to desk work typically happens within a week for most men. Physical labor and exercise should wait longer – generally 2 to 3 weeks. Sexual activity is typically resumed after 3-4 weeks, though the urologist’s specific guidance takes precedence based on how the procedure went.
The follow-up semen analysis, which shows whether sperm have returned to the ejaculate, is performed at approximately 6-8 weeks post-procedure. Because it can take several months for sperm parameters to stabilize and reach their best values after reversal, a single post-operative analysis showing low counts or motility doesn’t necessarily mean the procedure failed. Serial semen analyses over the months following reversal give a more complete picture.
Why Microsurgical Training and Surgeon Volume Matter
Vasectomy reversal is technically demanding. The structures involved are small, the sutures are fine, and the precision of the connection directly affects whether it remains patent. A surgeon who performs reversals occasionally in a general urology practice has a different cumulative experience than one for whom the procedure represents a meaningful portion of their surgical volume.
The in-office operating room at Lazare Urology is equipped and staffed specifically to support procedures that require the precision and conditions that vasectomy reversal demands – including microsurgical capability, the sedation team, and the post-operative support that makes the experience manageable for men coming from throughout the New York area.
Scheduling a Reversal Consultation at Lazare Urology
If you had a vasectomy and are now considering reversal, the consultation is where the realistic picture takes shape. Dr. Lazare reviews your vasectomy history, discusses the intraoperative variables that will determine which procedure is appropriate, and helps you understand what the outcomes data means for your specific situation – including an honest conversation about the role of your partner’s fertility in the overall equation.
Contact Lazare Urology to schedule a consultation. The office serves patients from Brooklyn, Manhattan, Queens, the Bronx, and throughout the greater New York region, and the in-office surgical facility means the procedure itself can be scheduled without the logistics of a hospital or ambulatory surgery center.